One main consequence of life-long immunosuppression necessary in transplant recipients is a reduced immunity, which increases the risk of infection. Infections in organ transplant recipients can be of bacterial, fungal, or viral origin. They might be transferred with the transplanted organ, or be a consequence of the immunosuppressive treatment causing the transplant recipients to be more susceptible to infections from their surroundings or from quiet infections their own bodies are harboring.
Bacterial infections of the skin are commonly streptococcal or staphylococcal in origin. This is true in transplant recipients as well as the general population. Transplant recipients may develop many atypical infections due to their immunosuppression. Thus all possible infections should be evaluated by a physician, with cultures taken to evaluate the type of infection and the appropriate treatment.
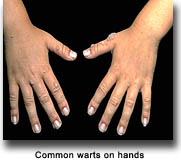
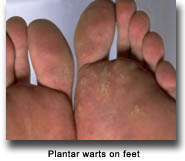
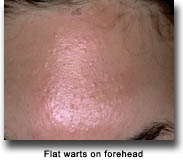
Warts are very common in transplant recipients, and may be seen in 50-85% of the recipients 5 years after the transplantation. Warts are a non-cancerous growth in the skin. Viruses in the family of Human Papillomavirus (HPV) can cause warts. There are greater than 100 different types of HPV. Most cause the same type of appearing warty type lesions. Few of these HPV types are associated with malignant degeneration and progression into a type of skin cancer. It is most often associated with squamous cell carcinoma. Warts appear as scaly white to pink to gray bumps on the skin. When occurring on the palms of hands or soles of feet they are known for interrupting the normal skin lines. They often have black dots noted throughout them, that some refer to as the "roots"; however, these are actually thrombosed capillaries. Warts can be very difficult to treat in transplant recipients. Current therapies for warts mainly depend on the destruction of affected skin areas. This destruction can be done with chemicals such as salicylic acid, cantharidin, 5-fluorouracil, and others. Physical destruction with liquid nitrogen, laser, curettage, or excision is commonly used. Immunomodulatory creams and injections can be used. Repetitive treatment is often required for ultimate success.
Herpes virus infections are important after organ transplantation, as they can be responsible for significant morbidity (poor life quality) and mortality (death) rates. The herpes viruses family includes different types of viruses such as cytomegalovirus (CMV), herpes simplex virus (HSV), Epstein-Barr virus (EBV), and varicella-zoster virus (VZV). These all have one distinct attribute in common: After the initial infection the virus lays dormant in the nerves, and, under certain conditions, may reactivate causing symptoms. There is no available treatment that will eradicate the viruses from the human body.
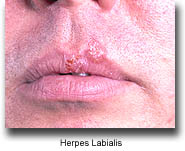
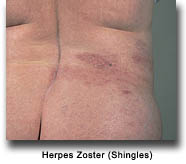
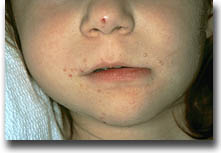
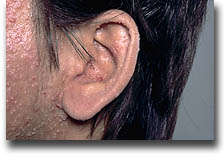
Herpes simplex virus (HSV) is the cause of cold sores and genital herpes. It is not to be confused with herpes zoster (commonly known as 'shingles') or herpes varicella (commonly known as 'chickenpox'), both caused by varicella zoster virus (VZV). Other types of herpes viruses are cytomegalovirus (CMV) and Epstein-Barr virus (EBV). EBV causes kissing diseases (infectious mononucleosis), but under immunosuppression, tumors of the lymphatic system can occur as a result of this virus.
Nearly 40% of the organ transplant recipients develop an infection with herpes viruses after 10 years of immunosuppressive treatment. HSV and VZV are responsible for many skin infections. HSV causes mucocutaneous lesions in more that 50% of the patients within the first 5 weeks after transplantation. Within 6 months after transplantation in 15% of the patient, a herpes zoster infection (VZV) has been documented. In the early post-transplant period there may be severe, eventually life-threatening infections with these viruses.
Herpes simplex virus tends to affect those parts of the body where two different skin surfaces meet, namely the angles of the mouth, the genital area, the rectum or anus and the eye. However, in immunosuppressed patients, the virus may affect other parts of the body or may persist as chronic herpetic lesions. Reliable and early diagnosis is crucial to initiating therapy in a timely fashion so as to prevent generalized infections.
Currently, drugs with anti-herpes virus efficacy, such as acyclovir and valacyclovir, are available and indicated for treatment of HSV and VZV. Many herpes virus infections in transplant recipients require oral or intravenous medication to adequately treat. People who experience recurrences may take continuous treatment to reduce the frequency of the recurrences. Early after transplantation, prophylaxis with antiviral medication is often prescribed.
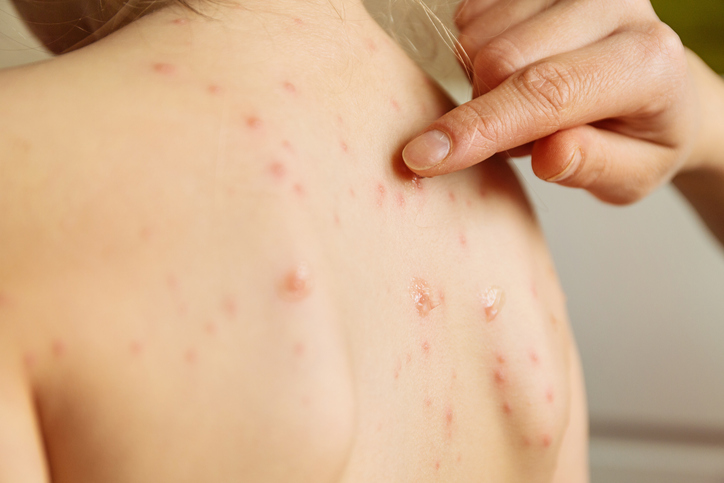
Molluscum Contagiosum is a noncancerous skin growth caused by a virus infecting the top layers of the skin. It is similar to a wart, but caused by a different virus. The virus causing this skin growth belongs to the poxvirus family. The virus is spread by skin contact and enters through breaks in the skin or hair follicles. It affects only skin, not internal organs. Molluscum appears as flesh colored/pink, dome-shaped bumps on the skin, often with a central indentation. They often appear in clusters. They may affect any area of skin. In patients on immunosuppression they may become quite large. Many dermatologists recommend treating molluscum because they often spread from one skin surface area to another. In the general population molluscum can resolve on their own after six months to 5 years. In the transplant population, these growths are more persistent because of the suppressed immune system that normally rids of this viral growth. Molluscum may be treated in many different ways. Treatment with liquid nitrogen is very common. They may be treated by various other methods, including: topical creams such as a retinoid or a topical immune response modifier, blistering agents, electric needle (electrocautery), or scraped off with a sharp instrument, such a curette. Treatment is determined on an individual basis.
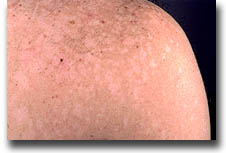
Tinea Versicolor is a common skin condition that is caused by an overgrowth of fungus that normally resides on our skin. This overgrowth results in uneven skin color and sometimes scale. It is usually completely without symptoms, but occasionally can be itchy. It most commonly appears as white-to-pink-to-tan-to-dark-brown spots on the skin of the neck, upper back, shoulders, and chest. It is more common in warm/moist seasons and climates. Transplant recipients are more prone to getting Tinea Versicolor due to their immunosuppression. It is generally not an infection that will make you ill. It is diagnosed when examination of a skin scrapping under the microscope shows fungus.
It is treated with either topical or oral medications. In transplant recipients, treatment with oral medication is avoided if possible, secondary to the potential drug interactions with their immunosuppressive medications and side effects of the oral antifungals. Topical selenium sulfide or topical antifungal creams are commonly used and found very effective. Tinea versicolor commonly reoccurs. To prevent recurrences, treatment with topical selenium sulfide once to twice a month is often effective.
This is a fungal infection of the nails. This more commonly affects the toenails than the fingernails. Infected nails appear thick, discolored (often yellow or brown), and with crusty debris under the nail edge or on top of the nail. These nails can be difficult to cut and can cause irritation to the skin around them. This is a very common infection. Infection of the nails with fungus can be difficult to treat. Treatment often requires an oral antifungal medication. In transplant recipients these medications have to be used with great caution due to their risk of drug interaction with the immunosuppressive medications the transplant recipient is taking, and due to the side effects of the antifungal medication on the liver. Treatment with topical antifungal creams is not effective for treatment of the nail. There are medicated nail polishes available with few side effects.
Recommended steps to control fungus are as follows:
Thick nails can be difficult to care for. It is recommended that the toenails be cut straight across, so as to avoid ingrown nails and pain. Routine toenail trimming by a podiatrist may be very beneficial.
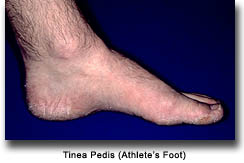
This is a fungal infection of the feet, often referred to as athlete’s foot. Affected feet are often itchy. The sole of the foot will appear red with scale and occasional vesicles (small bubbles just under the skin surface). The space between the toes is commonly involved with accumulation of white appearing scale and occasional small sores. It is diagnosed when examination of a skin scrapping under the microscope shows fungus.
This can generally be treated with over the counter antifungal creams used regularly. Some cases will require evaluation and treatment by your physician. Care should be taken to control re-infection. See recommended steps to control fungus, listed above in the onychomycosis section.
This is a fungal infection of the groin. It is characterized by red, scaly skin that can become "raw". It is often very itchy and can burn, if very irritated. It is diagnosed when examination of a skin scrapping under the microscope shows fungus. It is treated with topical antifungal creams. It is important to keep this area very dry by toweling dry after a shower and then using a cool blow dryer or fan to the area. Loose fitting clothing helps to avoid excess irritation.
